Stories

“I’m a living testimony of cataract surgery”
When Angeshita regained her independence after her eye operation, so did her family. They are now able to return to school and work, giving them all hope for the future.

Alinafe cuts the queues
Learn about one man's mission to make a difference in Malawi by training as an eye health specialist.

Bringing eye health into the classroom
Zahra is one of the many children now thriving thanks to a Sightsavers programme to screen school students for eye conditions and health problems.

Our sights are set on eliminating trachoma in Kenya
Four-year-old Lanoi was suffering with trachoma. With the help of eye health workers and volunteers, she received treatment to end the pain of trachoma.

Trachoma elimination in Benin: “All the pain was gone. It was like a miracle!”
Benin has become the latest country to eliminate blinding trachoma. Here we meet people whose lives have been transformed, and those who helped to banish the disease.
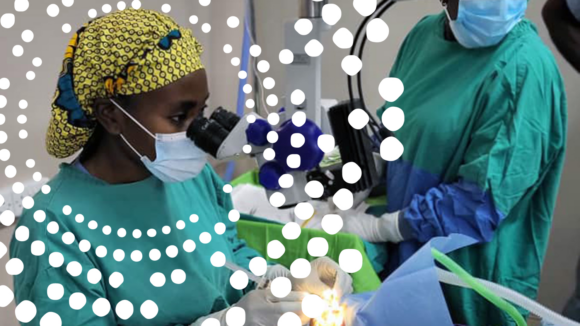
A day in the life: “You really feel that you’ve made a difference”
Dr Moira Chinthambi received a Sightsavers scholarship to train as an ophthalmologist and now works on our inclusive eye health programme in Malawi.

A day in the life: “I’ve wanted to do this for a long time”
Alinafe Zaina is studying clinical ophthalmology in Malawi with the help of a scholarship provided by Sightsavers’ inclusive eye health programme.

We are… promoting inclusive elections
We’re working with partners in Cameroon and Senegal to ensure people with disabilities are able to take part in every stage of the political process.
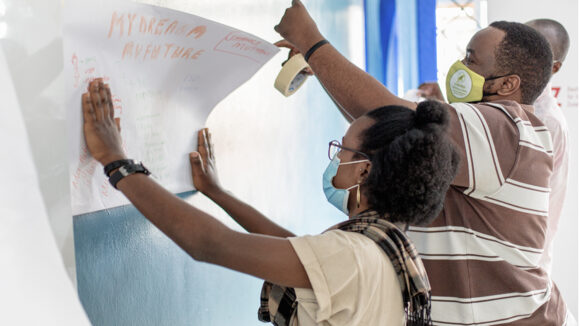
We are… training young people with disabilities
We’re working with partners in Kenya to give young people the skills and practical experience they need to begin a career in IT.

We are… creating inclusive eye health services
We’re working with governments in Uganda and Malawi to improve access to quality eye care services and prevent avoidable blindness.